CMS’s coding intensity
adjustment, which is used to account for the estimated difference between risk
scores that hypothetical beneficiaries would receive if enrolled in Medicare
Advantage vs. fee-for-service (FFS) Medicare, has led to more than $91 billion
in payments to MA plans between 2007 and 2022, asserted a March 3 letter from the Medicare Payment Advisory
Commission (MedPAC) to CMS Administrator Chiquita Brooks-LaSure. The agency in
its 2023 Advance Notice proposed
to use the statutory minimum adjustment of 5.9%, which MedPAC estimated will
lead to an inflated $16.2 billion in payments — and that’s on the conservative
end, the commission noted. MedPAC first raised this issue in 2016, when it
urged CMS to consider a new model that would use two years of FFS and MA
diagnostic data, exclude diagnoses documented only on health risk assessments
from either MA or FFS, and then apply an adjustment that fully accounts for the
remaining coding differences. The commission in its March letter reiterated its
support for this approach.
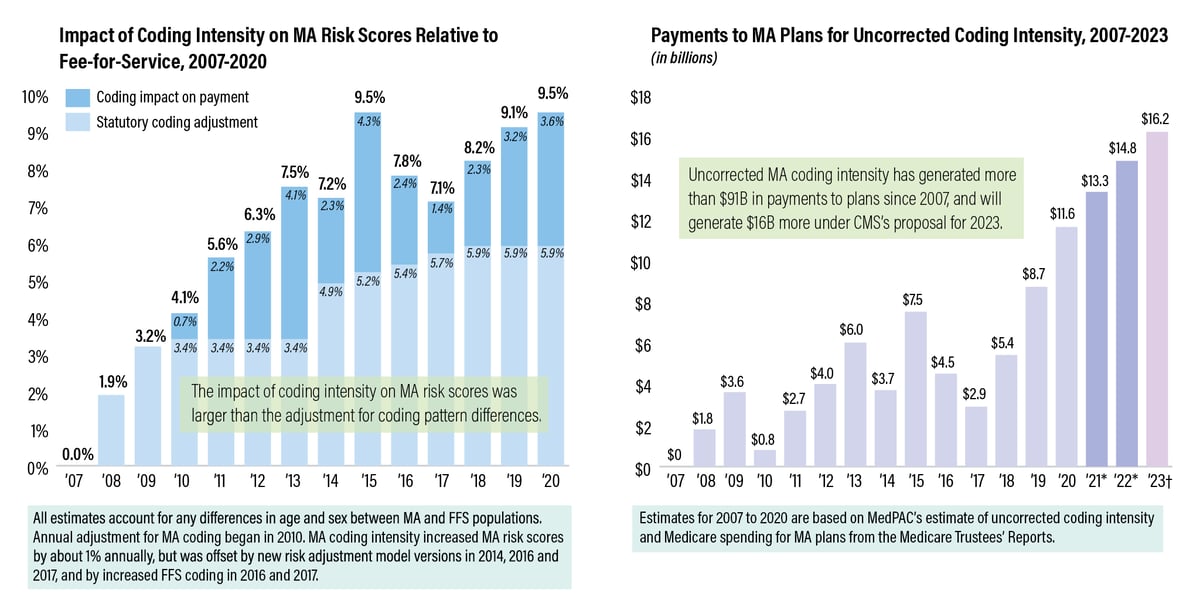
*Conservative
estimates assume that coding intensity will remain at 3.6% and are based on
projected Medicare spending for MA plans from the 2021 Trustees’ Report.
†Conservative
estimate assumes coding intensity will remain at 3.6%, is based on projected
Medicare spending for MA plans from the 2021 Trustees’ Report and assumes CMS
will apply the proposed 5.9% coding adjustment.
SOURCE: MedPAC analysis of CMS enrollment, risk score files
and Medicare Trustee’s Reports, 2019-2021, March 2022.
No comments:
Post a Comment